 
Furthermore, to avoid selection of resistant strains and subsequent treatment failure, initial treatment should include bacterial load-independent drugs with low risk of resistance development, such as β-lactams, vancomycin or daptomycin. Although the bacterial load is reduced by surgery, high-dose antibiotics and optimization of PK/PD parameters achieve better infection control and lower the risk of bacterial resistance emergence. 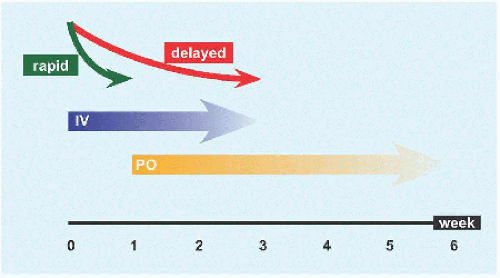
PJI treatment requires optimal antibiotic coverage, especially during the early phase, i.e., the first postoperative weeks. Initial IV Antibiotics and Extended Infusion Two very different surgical strategies are applied, depending on the clinical picture: prosthesis retention with débridement, synovectomy and exchange of the mobile elements for acute infection, while biofilm formation is still ongoing or prosthesis removal followed by a new arthroplasty during one- or two-stage exchange for chronic infections.Ģ. Optimal curative treatment of PJI combines surgery and prolonged, high-dose, antibiotic therapy. Precise identification of the microorganism(s) and their antibiotic susceptibilities are crucial to successfully treating these patients. It brings together recent findings on the subject and the extensive experience of our reference center for complex bone and joint infections.Ĭlinical diagnosis of PJIs can be challenging because of the indolent course of chronic infections, difficulties culturing low-virulence bacteria, and the wide variety of microorganisms and antibiotic-resistant phenotypes that can be involved. Herein, we first develop more practical aspects and key points of antibiotic therapy for PJIs, and then detail the specific management of various microorganisms. This review is not intended to be a substitute for those guidelines. Indeed, the number of high-evidence studies to support a specific recommendation was limited and diverse practice patterns for a given clinical setting seemed to obtain similar outcomes. As stressed in the guidelines introduction, many of those recommendations were based on expert opinions. International guidelines were published nearly 10 years ago. Their efficacy is highly dependent on the choice and quality of the surgical procedure, and on the quality of the microbiological diagnosis. Antibiotics represent only a part of PJI management and are closely linked to the surgical strategy applied. A multidisciplinary approach, with strong collaboration among all medical and surgical personnel involved, is essential. 
PJI treatment is complex because it deals with a large number of different clinical contexts, relying on specific surgical and medical strategies, which have to be adapted to the patient. That rate is much higher for revision arthroplasty, reaching up to 15%. The PJI rate is 0.5–2% for primary knee, hip and shoulder replacements. This operation also carries risks, however, among which prosthetic joint infection (PJI) is the most severe, carrying a high economic and human burden. It is estimated that, by 2050, this number will increase 42–112.3%. Nearly 200,000 total hip replacements are performed annually in France. Joint arthroplasty is now a very common and successful surgical procedure to restore joint function. Herein, we address PJI management based on recent literature data, guidelines and the experience of our referral center for complex bone-and-joint infections. Choosing the optimal agent(s) is one aspect, with others being optimization of drugs’ pharmacokinetic/pharmacodynamic parameters, the choice of administration route, use of monotherapy or combination regimens, therapeutic drug-monitoring and patient education to improve compliance and tolerance. Although guidelines have been published, many aspects of antibiotic therapy remain poorly established. Their efficacy depends to a large extent on the choice and quality of the surgical procedure, and the quality of the microbiological diagnosis. Antibiotics are only one part of the therapeutic regimen and are closely related to the surgical strategy. Its management combines surgical intervention, whose type depends on the clinical situation, and prolonged high-dose antibiotics adapted to the responsible microorganism(s) and the patient. Prosthetic joint infection (PJI) is a severe complication after arthroplasty. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
